I’ll never forget the day I woke up feeling as though I was experiencing a heart attack. My clothes were drenched all the way through with sweat and I had tremors down the right side of my body. I called my partner to tell him I wasn’t feeling well. He had told me to lie down, rest for a bit but as I ended the call I still felt like something was wrong.
Not long after, I started experiencing heart palpitations. My heart began to pound quicker and skipped every few beats. I hit redial and told him I thought I was having a heart attack. He told me he would be calling an ambulance and hung up. Every minute felt like an hour as I waited for them to arrive.
Whilst I waited, I wrote an SMS to everyone in my family –
“I think I’m having a heart attack, I called an ambulance. I love you.”
It sounds dramatic, I know! I had dealt with sinus tachycardia and atrial fibrillation since I was 19 but nothing this extreme. When I look back at the ordeal, I still get upset thinking about it. I’m terrified of falling asleep and waking up in a similar state.
After a 15 minute wait, the paramedics arrived and the next thing I know I’m being strapped in, pushed into an ambulance, and we’re on our way to the hospital.
This was not the first hospital visit during the ordeal. Two days earlier I was in the ER. I had been ill for a week with a fever, dizziness, skin discoloration, weight and muscle loss with extreme fatigue. I was lying on the couch when I lost complete movement of my legs. I practically begged my partner to drive me to the hospital. When I arrived, I could barely walk to the triage station. After blood work, an external and internal pelvic ultrasound and an IV infusion later, the result – you have a nasty virus and wait it out. You’re having an allergic reaction to penicillin. Stop and ask for an alternative antibiotic from your doctor. I left that night completely disheartened. I knew what an allergic reaction to medicine felt like, I had experienced it before, and this was not it.
After arriving in the ambulance during the second visit, x-rays were conducted and again the hospital did not find anything wrong with my bloods. They repeated what they had mentioned a few days beforehand, that I was fighting an “infection”. The only thing they found concerning was that my heart rate would spike whenever I moved – drinking water, sitting up, talking. I was sent home after a few hours and told to see a cardiologist as soon as possible just to double check if the infection had reached my heart.
The photos below are only 3 months apart. December 2015 and March 2016. In the weeks leading up to my hospitalisation, I had lost 10kg (20 pounds).

Two days later, I found myself in ER for the third time experiencing the same symptoms. Muscle weakness, heart complications, fever and low blood pressure. It was during this third visit, that I realised the hospital had done everything they could. The doctors were no different. I had visited 6 GP’s – all of which could not figure out the cause of my symptoms. Having exhausted all avenues with the GP’s, I was sent to a professor associated with the medical centre and the process of figuring out what was wrong with me began.
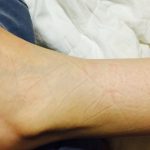
From mid-February to early March, I continued to drastically lose weight. The photo below is of the actual size and colour of my lower legs during the worst of my illness. My legs were the size of my arms and I was unable to walk without assistance.
I have to admit, this whole event wasn’t a surprise to me. In the back of my mind there was this unnerving feeling something was eventually going to happen. It wasn’t as though I had been symptom free and all of a sudden this had occurred. For three years I had been visiting doctors complaining of extreme exhaustion. When I say exhaustion, I don’t mean tired. Tired is when you go to bed and wake up in the morning refreshed. I was going to bed and sleeping 5/6 hours a night regularly and when it was really bad – 15 hours overnight. I’d wake up worse than when I went to bed. I felt nauseated, my muscles ached and there was this weighted feeling on my chest. It was an unusual exhaustion. I would walk down the road, a simple 5 minute walk and end up feeling as though I was about to collapse. As a manager, I struggled to hold team meetings as I suffered from breathlessness. Sounds began to disorient me and I became extremely sensitive to sunlight. When I explained this to my doctors they would laugh it off and say ‘look at your work hours – that’s why you’re tired. You need to change your job because this stress is going to lead to a breakdown.’ I’d beg for blood work to be done and it would all come back normal – the only deficiencies were in vitamin D, zinc and B12. Nothing major.
It took a devastating breakdown like this to make me understand my body better. For years I had just gone along with what I was being told, you’re stressed, you need more sleep, you must be depressed. But now, as they stared back at me and said ‘you may never find out the cause of your illness. Just be glad it’s stabilising’, I knew I couldn’t settle for that explanation. I wasn’t going to sit around and wait for the next hospitalisation before I was hit with another reality check. I strove to really become my own advocate for health – pushing for referrals to the right specialists, changing specialists if they were not offering the best assistance, improving my diet, researching natural remedies to improve chances of remission. It was now my responsibility to take charge of my health and ensure I received the answers I was looking for.
The professor I mentioned earlier played a big part in my recovery. It may have taken a few years and hospitalisation for me to learn of my autoimmune disease but I’ve heard of many people waiting decades to find out. He dissected each of my symptoms and created his own team of experts to assist with helping me find out what was going on. In future blogs I’d love to discuss my experiences with my endocrinologists, immunologist, cardiologist. Actually, there’s quite a few topics I’d love to focus on within this blog – removing toxins, dealing with finance management when you have medical expenses, learning to enjoy life through the every day pain – there’s just so much I’ve already experienced on my road to recovery.
As of February 2017, my thyroid antibodies have dropped to being within the normal range – which I think was due to a change in diet and stress management. I’m working on maintaining control over my autoimmune diseases and learning to live an intentional life. It was a devastating shock initially but behind it all I find my diagnosis a blessing. It’s made me rethink exactly what was important in life and forced me to take more of an interest in my personal health.
Remission doesn’t happen overnight, it requires a complete overhaul of your lifestyle. Anything can trigger flares and exacerbate symptoms and I want to share with you my strategies for minimising the unnecessary stress in life that contributes to inflammation in the body. I’d also love to hear your experiences and lifestyle tips too! If you’re comfortable with sharing your story please comment below or send me an email at laura@liveminimal.com.
In my next blog post, My Autoimmune Journey Part 2 , I’ll be discussing the factors I believe were behind triggering my autoimmune diseases.